Last Updated on April 5, 2026 by Dr. Nico Kamosi
Introduction
Full mouth rehabilitation represents one of the most complex and challenging endeavours in modern restorative dentistry. It is strongly indicated in patients with severe, advanced bone loss, gum recession, or other disease processes that render the prognosis of remaining teeth poor and subject to extraction. It is also essential for patients suffering from severe grinding and clenching, which causes fracture and destruction of tooth structure. When patients have lost some teeth due to gum disease but retain some salvageable teeth, full mouth rehabilitation addresses both restorative function and aesthetics in the context of compromised oral function.
The comprehensive restorative approach integrates the applied science of biomechanics, tissue engineering, and biomaterials to restore teeth and, most importantly, to improve the quality of life in people suffering from compromised function and deteriorated appearance.
The modern era of full mouth rehabilitation has been transformed by recent advances in implantology, laboratory technology, and biomaterials. These developments enable us to approach each clinical case holistically and implement the most desirable atraumatic restoration techniques. This requires meticulous treatment planning, compatible material selection, advanced laboratory techniques, and effective patient communication through a multidisciplinary clinical approach.
This article will discuss the indications and contraindications for full mouth rehabilitation, contemporary methodologies, material considerations, and the pivotal contribution of the experienced dental technician in achieving optimal outcomes.
Clinical Indications and Contraindications
Indications for Full Mouth Rehabilitation
- In partially edentulous or fully edentulous patients with multiple missing teeth, severe surface wear, non-salvageable chronically periodontally involved teeth, or multiple mobile teeth
- In individuals with significant aesthetic problems affecting quality of life
- Patients with a history of tooth structure loss due to parafunctional habits, clenching, or bruxism
- Patients with systemic health conditions that deteriorate periodontal health, such as diabetes or immunocompromised states, who require holistic rehabilitation strategies
Contraindications and Cautions
Contraindications and Cautions
- Uncontrolled systemic diseases, particularly diabetes and bone metabolism disorders
Severe - immunocompromise
Relative Contraindications:
- Unmanaged periodontal disease
- Poor oral hygiene motivation
- Significant financial constraints
- Lack of intellectual or emotional understanding, poor patient acceptance, psychological barriers, or unrealistic expectations, which render the treatment complex and unpredictable
Additional Considerations:
- Untreated parafunctional habits may lead to biomechanical complications such as implant infrastructure failure and temporomandibular joint dysfunction
- Active smoking adversely impacts the long-term prognosis of full mouth rehabilitation, especially in patients with other immunological disorders or dysfunction. Smoking compromises the health of the supporting tissues and the long-term stability of restorations. It is therefore essential to discuss the adverse impact of smoking on the success and survival of restored and rehabilitated dentitions before embarking on complex treatment strategies.
Modern Treatment Methodologies
Tooth-Supported Restorations
Tooth-supported restorations, utilizing partial dentures or fixed crown-and-bridge restorations, have long been considered the gold standard for maintaining natural root proprioception. However, missing teeth may lead to varying degrees of alveolar bone resorption.
Fixed crown-and-bridge restorations provide superior tactile feedback and aesthetic outcomes, especially when utilizing modern adhesive techniques and minimally invasive preparations.
The use of minimal tooth preparation protocols, metal-free core build-up materials, posts, and fibre-reinforced composites has revolutionized advanced reconstructive dentistry. These innovations extend the lifespan of severely compromised teeth through conservative preparation approaches.
Implant-Supported Restorations
Over the last four decades, dental implants have progressively revolutionized full mouth rehabilitation, offering predictable long-term treatment strategies in edentulous or partially edentulous patients.
Implant-supported crowns, fixed bridges, and removable prosthetics supported on osseointegrated dental implants provide superior functional and aesthetic outcomes when compared to conventional removable dentures.
Although titanium implants remain the gold standard with osseointegration rates exceeding 95%, the advent of novel ceramic implants offers significant advantages. Ceramic implants provide superior biocompatibility and are the ultimate biocompatible material. Care must be taken to understand ceramic implant behaviour and ensure careful case selection to avoid biomechanical failures in patients with severe grinding habits, professional loading activities, occlusal discrepancies, or increased mobility.
Combined Tooth and Implant Support
The strategic preservation of remaining natural teeth while placing dental implants through combined tooth and implant-supported restorations offers the most desirable versatility and clinical outcomes. This combination, however, requires extensive knowledge of biomechanics and materials, complex prosthetic execution, occlusal principles, and careful material selection.
It is essential to design prosthetic restorations to distribute forces equally on supporting teeth and implants. This requires extensive knowledge of the periodontal ligament and support mechanisms, particularly in individuals with compromised or critical support.
The discrepancies in biomechanical and physical properties between tooth and implant materials, when combined in sophisticated prosthodontic arrangements, require high-quality technical execution.
Material Selection and Innovation
Traditional Ceramic and Metal Systems
Metal and gold-based restorations remain the gold standard for mechanical longevity, offering adequate marginal adaptation. Porcelain fused to metal (PFM) restorations provide good aesthetic outcomes with proven long-term clinical success when properly executed. However, the disadvantages of metal visibility and occasional biological reactions in individuals allergic to base metals have shifted clinical preference towards all-ceramic systems.
All-Ceramic and Zirconia Systems
Modern high-strength zirconia materials have revolutionized advanced restorative dentistry by providing exceptional strength, superior aesthetics, and most importantly, excellent biocompatibility with reduced plaque adhesion.
Lithium disilicate and leucite-reinforced ceramics are ideal materials for full mouth rehabilitation, offering both aesthetic properties and excellent marginal precision. These materials are suitable for both tooth-supported and implant-supported restorations, providing multiple clinical advantages.
Zirconia Implants: A Paradigm Shift
Over the past decade, zirconia implants have been introduced as an alternative to titanium implants, with particular value in specific clinical contexts.
Patients with metal allergies or titanium sensitivities can tolerate zirconia implants well. Zirconia implants eliminate metal visibility in the aesthetic zone, providing superior aesthetic properties and biological advantages through reduced plaque accumulation and inflammatory response compared to titanium.
While some literature suggests zirconia implants demonstrate lower osseointegration rates (approximately 80–90%), other evidence indicates that success rates can be comparable to titanium implants. Zirconia implants are indicated in highly selected cases and specific patient populations, particularly in the upper anterior region requiring maximum aesthetics and in patients with metal sensitivities, where they offer superior advantages.
The Indispensable Role of the Dental Technician
The dental technician is a critical member of the multidisciplinary team in the reconstruction of missing teeth. Working in collaboration with the implant surgeon and restorative prosthodontist, the dental technician brings specialized expertise essential for managing the complexity of full mouth rehabilitation cases.
The dental technician possesses deep expertise in occlusal science, biomechanics, and the chemical, physical, and mechanical properties of materials. They have mastered digital prosthodontic design technologies, material science, and biomechanical principles.
Therefore, it is essential to establish efficient communication between the triad of surgical implantologist, prosthodontist, and laboratory technician to clarify the specifications of all prosthetics from both technical and aesthetic perspectives.
Having a proficient dental technician as a long-term partnership facilitates clinical decision-making and the execution of prosthetic devices and workflow.
The Modern Approach: Digital Integration and Holism
In contemporary full mouth rehabilitation, a myriad of novel digital technologies—including intraoral scanning, cone-beam computed tomography (CBCT), and computer-aided design and manufacturing (CAD-CAM)—are progressively integrated into full rehabilitation protocols.
In recent years, precise surgical planning and predictable aesthetic and functional outcomes have enabled clinicians and laboratories to achieve significant improvements in the quality of life of well-selected patients, in terms of nutritional status, sleep quality, stress reduction, and systemic health improvement.
Practitioners increasingly understand that compromised mastication from tooth loss impairs nutritional intake and that restoration of function profoundly improves overall health and quality of life. This biologically informed paradigm positions dentistry as integral to systemic health management.
Benefits of Tooth-Supported and Implant-Supported Combinations
The concept of full mouth rehabilitation through combined tooth-supported and implant-supported prosthetics offers synergistic advantages that maximize reciprocal support between remaining natural teeth and dental implants.
This approach leads to superior masticatory efficiency by engaging proprioception from retained natural teeth, thereby protecting implants from untoward mechanical overloading and resulting in improved longevity of both natural tooth and implant restorations.
Additionally, patients benefit from a financial advantage by avoiding the need for more implants than necessary, making comprehensive treatment more accessible and affordable.
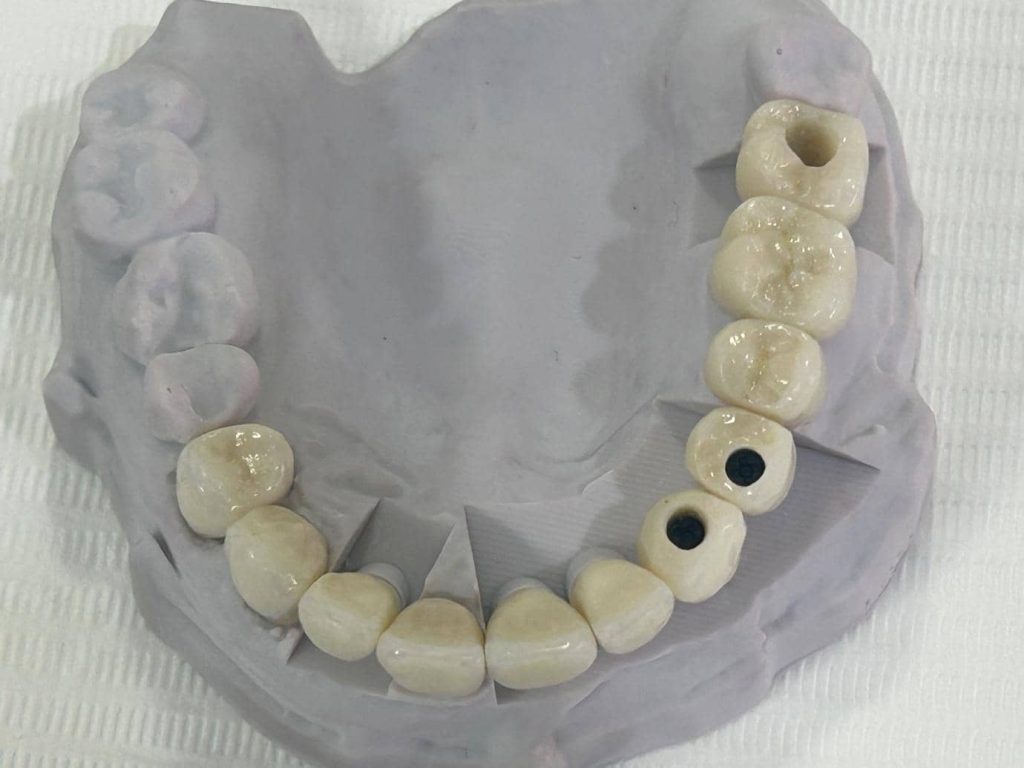
Clinical Case Example
Patient Background
A 52-year-old patient presented with a severely compromised dentition: failing root canals in teeth #7, #5, #4, #2, #1 (upper left and right regions), with remaining teeth presenting fractured crowns, extensive fillings and caries, localised bone loss from chronic periodontitis, and significant occlusal discrepancy.
The patient was concerned about declining chewing function, increasing difficulty in consuming a normal diet, and was losing confidence due to her unpleasant dental appearance. Comprehensive treatment planning identified her as an ideal candidate for combined tooth-supported and implant-supported rehabilitation.
Treatment Strategy
The treatment plan incorporated a combination of single-tooth implant-supported crowns (zirconia-supported) and tooth-supported single crowns in both anterior and posterior regions. Bone augmentation was performed to create adequate quality and quantity of bone around the implants supporting the crowns.
The crowns supported by natural teeth were designed independently of those supported by dental implants, as the biomechanical principles and support mechanisms differ significantly.
This case was managed through a multidisciplinary approach to maximize aesthetic and functional outcomes while enhancing the overall biomechanical capability of the prosthetics in distributing functional loading appropriately. Strategic zirconia implant placements coupled with retained and treated natural teeth provided the foundation for both anterior and posterior support using high-quality aesthetic E-max crowns.
Outcomes
At 18-month follow-up, all implants demonstrated excellent osseointegration, the natural teeth remained vital and stable, and the patient reported significantly improved chewing function, diet quality, appearance, and psychological well-being.
Conclusion
The multidisciplinary execution of full mouth rehabilitation requires a sophisticated combination of surgical, prosthetic, technical, and restorative expertise. Success demands comprehensive treatment planning, patient communication, meticulous patient selection, appropriate material selection, advanced technical design and execution expertise, and above all, a commitment to holistic patient care.
We have the privilege of accessing advanced technological innovations and novel biomaterials that enable clinicians to achieve outcomes previously unattainable. The integration of both zirconia and titanium implants along with natural teeth supporting durable zirconia and E-Max crowns provides our patients with long-lasting restorations that improve mastication and comfort while substantially enhancing their overall quality of life.
Dr. Nico Kamosi

Dr. Nico Kamosi
Specialist Periodontist, Implantologist, Prosthodontist, Holistic and Biological Dentist
TDL. DDS. (Swe.), MSc.Perio.(Eng.),
MClinDent.Perio.(Eng.), MSc.Imp.Dent.(Eng.),
Dip.Aesth.Med. (Eng.), MClinDent.Prosth.(Eng.),
Cert., Dip.DHSLM.(RCS.Eng.), Cert.Orth.(Eng.), Cert.Law (Eng.), AIAOMT
Accredited member of IAOMT, SMART Certified
Member of AACD, EFP, AAP, ESCI, IAOMT

