What is Guided Bone Regeneration?
As a result of tooth extraction, dental infection, trauma and post-operative bone resorption, it would be necessary to reconstruct or augment the bony ridge defect around the missing teeth prior to or simultaneous to implant placement to ensure that there is sufficient bone around the implant.
Why Bone Augmentation Is Critical
The function and the aesthetics of implant-supported teeth can be severely compromised when the supporting bone and gum are deficient. Replacing a lost tooth with an implant-supported crown option is impossible in the absence of intact bone.
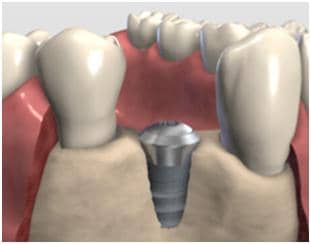
Exposed implant due to the localised bone resorption.
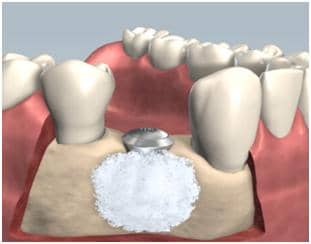
Bone regenerative procedure using bone graft material.

Causes Of Pathological Bone Loss
Periodontal Disease – the crestal and lateral aspects of bone walls collapse rendering deficient bone ridge architecture which provides inadequate implant support.
Root Canal Necrosis and Apical Infection – apical infections destroy lateral and apical bone periphery walls while sinus floor may become infected and lose integrity.
Bone Resorption After Extraction
About 50% of alveolar socket bone ridge width resorption occurs during the first year, with highest resorption rate in first 3 months (average 1mm). Bone resorption occurs more extensively horizontally around the buccal bundle bone and anterior teeth as buccal bone plate is thinner than lingual side.
Factors Affecting Resorption Rate
- Traumatic nature of root elevation and flap type (split vs full thickness)
- Systemic and local biological health of patient
- Patient lifestyle such as smoking
- Number of roots
- Pre-extraction dimensions of peripheral alveolar bone
- Hard and soft tissue biotype
What Is Guided Bone Regeneration?
GBR is a technique to reconstruct and restore bone deficiencies using a resorbable or non-resorbable membrane acting as biological barrier. This promotes bone cell ingrowth and mineralisation while preventing soft-tissue cells from entering the defect.
Guided bone regeneration uses various techniques and materials including human/animal-derived and synthetic products. Based on amount of bone required, patient’s bone or mixture of materials may be used.
In the absence of GBR, undermined or deficit gum may develop further into exposure of implant neck by untoward biological breakdown of surrounding tissues, causing aesthetic and biological complications such as peri-implant mucositis or Peri-implantitis.
Minor Bone Deficiencies
For minor bone deficiencies, GBR may be implemented with a membrane acting as biological barrier to promote bone regeneration and mineralisation. The barrier prevents other cells from growing into defect, enabling bone cell ingrowth.
Bone Regeneration Materials
AUTOGRAFTS
Human autogenous bone grafts can be harvested from upper or lower arches such as wisdom tooth or chin. Autogenous bone can also be collected during implant drilling procedures.
ALLOGRAFTS
Human bone grafts harvested from other human beings and processed from bone banks using live or cadaver bones. All allografts processed from donors negative by FDA-approved tests for HBsAg, anti-HBc, anti-HCV, STS, Anti-HIV and anti-HTLV-I. Although efforts made to ensure quality, most tissue banks make no claims concerning biological or biomechanical properties of provided allograft.
XENOGRAFTS
Bio-Oss is natural bone mineral derived from bovine (cow) bone with similar micro-architecture to human bone. Bio-Oss promotes bone scaffolding and has osteoconductive properties promoting ingrowth of blood vessels and bone cells which gradually integrate into native bone completely. Bio-Oss particles may remain in tissue bed surrounded by native natural bone.
ALLOPLASTS
Bone ceramic particulates such as Maxresorb or Regen are synthetic bone graft materials made from biphasic tri-calcium phosphate naturally present in our bone. Based on micro-porosity of particulated grafts, resorption profile varies from three to twenty months.
BIOLOGICAL MEMBRANES
Protective membranes could be non-resorbable (e-PTFE) or collagen membrane derived from porcine (pig) or bovine (cow) collagen. Membrane protects graft particulates within scaffold of bone defect periphery while preventing displacement and early resorption of graft material. Most collagen membranes resorb entirely by body following bone regeneration.
Important note: If you do not wish to consent to have any animal-derived graft or membrane products, please inform your doctor before signing consent forms.
Guided Bone Regeneration – Clinical Application
Guided bone regeneration or augmentation procedure may be performed by specialist periodontist using various techniques and materials including synthetic products and animal/human derived biomaterials. Based on amount of bone required and patient’s preference, one or mixture of bone replacement materials may be used.
Our experienced surgeons in London Specialist Dentists apply most scientifically approved material and techniques in field of Bone Regeneration throughout surgical procedures to improve long-term biological success.
CLINICAL EXPERTISE:
Dr. Kamosi specialises in advanced bone regeneration, guided bone regeneration (GBR), ridge preservation, sinus augmentation, and atraumatic tooth extraction. Expertise in surgical implantology and restorative prosthodontics enables him to deliver predictable outcomes in complex cases requiring bone augmentation and implant-supported restorations. Particularly skilled in full-mouth rehabilitation and aesthetic dentistry, combining biological principles with advanced surgical technique.

