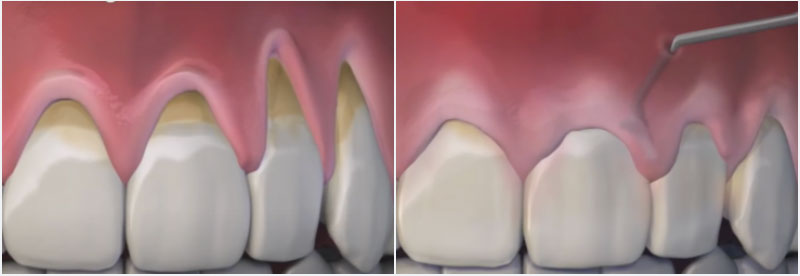
Most periodontal specialist or soft tissue plastic surgical protocols involve the correction of gum or mucogingival deficiencies and root coverage. Albeit, there is a need to optimise the currently implemented conventional treatment strategies to diminish the untoward postoperative surgical morbidity or discomfort, and optimise their clinical outcome.
The currently advocated minimally invasive surgical protocols have addressed some of the concerns for potential surgical trauma when regenerating the soft-tissue deficiencies and root exposure.
The modified Vestibular Incision Supra-periosteal Tunnel Access (M-VISTA) has been claimed to implement the principles of minimally invasive mucogingival surgery to optimise the treatment outcome and patient-reported outcome measurements (PROMs).
The recently well-published minimally invasive (M-VISTA) involve supra-periosteal key-hole access, tunnelling tissue bed preparation, and soft tissue graft stabilisation.
The M-VISTA technique is claimed to reduce surgical time and increase patient comfort by preventing trauma to the periosteum and reducing the grafted connective tissue vascularity.
A tension-free coronally advanced supra-periosteal mucosal flap will preserve the structural and vascular integration of the papilla. as opposed to the non-autogenous graft, the connective tissue may enhance the zone of keratinization. In such procedures, graft stabilization is crucial for increased plasmatic perfusion and vascular circulation.
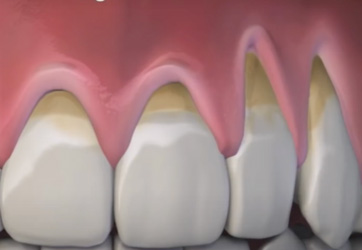
Miller Class II / Cairo RT1

Miller Class II / Cairo RT1
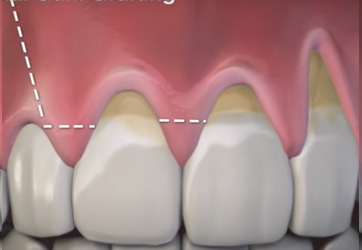
Incision and release of the mucoperiosteal flap
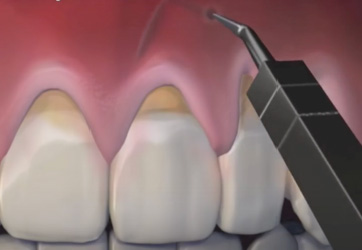
Tunnelling and release of the mucosal flap
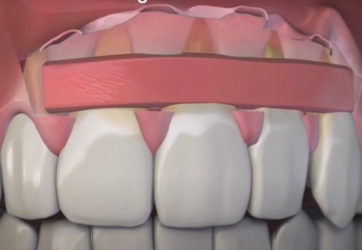
Flap elevation and CTG in-Situ
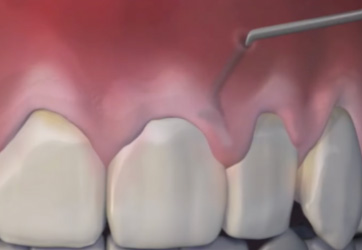
Tunnelling and coronal advanced flap
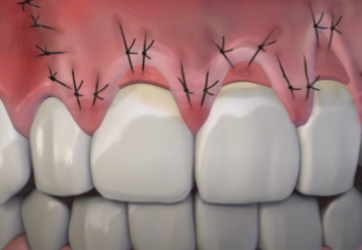
External suturing of advanced flap and CTG
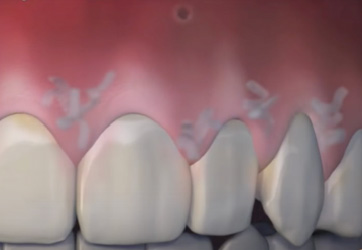
Internal stabilisation of advanced flap and CTG